Radiation and Chemo Therapy
Oral Cancer Treatments
Oral and Head and Neck cancers are a group of diseases. The common denominator is that dental management is required both prior to and after cancer treatments to enhance quality of life and minimize complications. The most common cancer treatments involve surgery, radiation and chemotherapy. These modalities are often combined. Hence, oral cancer patients generally are treated by a team of doctors. The purpose of this section is to provide a general overview of the dental treatment for patients who have been or will be treated with radiation, chemotherapy, combined chemo-radiation therapy, and those with surgical defects of the upper/lower jaws, tongue, and soft palate.
Head and Neck Radiation
Radiation therapy is routinely used to treat tumors of the head and neck. It may be used as the sole treatment modality. More often, it is combined with chemotherapy to treat certain cancers of the tongue, tonsil, and throat. Also, radiation is often used as an adjuvant therapy after surgery, i.e. post operative radiation therapy. The goal is to destroy tumors and microscopic disease, i.e. cancer cells in regional locations. Unfortunately, the radiation beam damages the healthy tissues it passes through on its way to the cancer. Generally, the areas affected are the salivary glands, upper and lower jaw bones where the roots of the teeth are located, soft tissues of the mouth and face, the muscles and jaw joints involved in opening and closing the mouth. The damage is generally dose dependent. Unfortunately many of the cancers are squamous cell carcinomas requiring high doses, 7,000 centigray for tumor control and 5,000 centigray for microscopic disease. In recent years, however, it has been possible to minimize the dose to collateral tissues with the advent of intensity modulated radiation therapy (IMRT). Generally, radiation therapy is given 5 days per week for five to eight weeks utilizing an external beam. Sometimes, radioactive seeds are placed directly into the tumor. This is called brachiotherapy. It delivers a high dose to the tumor and the hard and soft tissues in close proximity.
Complications/Side Effects
Dry Mouth (Xerostomia)
Radiation to the salivary glands causes fibrosis and cessation/alteration of salivary flow. As a result, teeth become more susceptible to decay (radiation caries), taste alteration occurs, and oral functions such as swallowing, chewing and speech become more difficult.
Decay of Teeth (Radiation Caries)
This is related to altered/reduced salivary flow. The saliva no longer has the protective qualities that naturally prevent tooth decay. To compensate, the dentition must be protected by the daily, indefinite use of fluoride, meticulous home care, and frequent dental cleanings.
Osteoradionecrosis (Destruction of Jaw Bone Secondary to Radiation)
It is a complex process caused by high doses of radiation therapy that damage the small blood vessels in the jaw bones. As a result, the jaw bones are unable to heal properly. It primarily occurs in the lower jaw in regions that have received a dose greater that 6,000 centigray. It can however, occur at lower dose levels. Infrequently, the upper jaw is affected. The risk increases over time. It rarely occurs during the first year after treatment. Patients treated with combined chemo/radiation therapy are particularly susceptible.
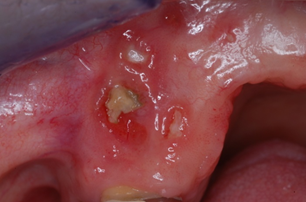
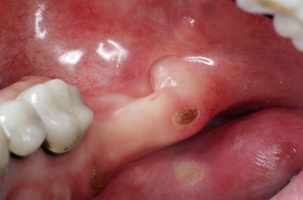
Mucositis
Mucositis refers to soreness of the internal soft tissues of the mouth: cheeks, tongue, palate and throat. Patients typically notice it several weeks into radiation treatment. Painful ulceration often occurs which increases the risk of infection. Generally it resolves within several months after completion of treatment.
Dysphagia
Dysphagia refers to diminished ability or inability to swallow both during and following radiation therapy secondary to mucositis and fibrosis of the mouth, throat, and other structures involved in swallowing. Some patients have stomach tubes placed prior to radiation or combined chemo/radiation anticipating the event that they will not be able to take adequate nutrition orally. Most often, dysphagia resolves within several months upon completion of radiation treatment. Swallowing therapy is indicated for refractory cases.
Restricted Opening of the Mouth (Trismus)
Contraction of the chewing muscles and capsules of the jaw joints occurs with unpredictable frequency and severity several months after completion of radiation therapy. There are certain surgical procedures that exacerbate trismus. Treatment for this problem is available.
Hypogeusia/Dysgeusia
Permanent taste loss may occur at a dose of 6,000 centigray if the tongue is in the high dose field. Below this dosage level, recovery usually takes several months. “Taste buds” on the dorsal (top) surface of the tongue that allow for discriminative taste acuity can be affected by mucosal ulceration that can last months to years.
Loss of Periodontal Attachment
Teeth in high dose areas tend to experience more profound loss of bone and soft tissue support.
Nutritional Deficiency
Nutritional deficiencies may occur as a result of mucositis, xerostomia, altered taste, and decreased appetite. Symptoms may include weight loss, dehydration, stomatitis, and oral infections such as thrush.
Dental Treatment
Before and During Radiation
Prior to oral cancer treatment, the patient should be evaluated by a dentist who has been formally trained to work as a member of a head and neck cancer treatment team, i.e. a Maxillofacial Prosthodontist. The status of the teeth, gums, bone support and the patient’s ability to maintain meticulous oral hygiene for the rest of their lives must be determined. Teeth with periodontal disease and advanced decay located in areas that are anticipated to receive a high dose of radiation should be removed. Ten to fourteen days of healing should be allowed prior to initiation of radiation therapy. Determining radiation doses to particular areas of the upper and lower jaws involves direct communication between the dentist and radiation oncologist. Restoration of decayed and broken teeth, smoothing of rough areas of teeth, and adjustment of ill fitting removable prostheses can be accomplished prior to or during the initial phase of radiation treatment. The teeth should be cleaned and a 3 month recall interval established with the dental hygienist. Fluoride therapy should be initiated. It may be accomplished in the following ways: carriers, prescription tooth paste, and brush on gel. Fluoride helps the tooth enamel resist decay. Patients must use fluoride for the remainder of their lives. It is generally necessary to repeat and reinforce fluoride therapy education prior to and following radiation therapy.
It is recommended that patients consult with their radiation oncologist about xerostomia (dry mouth) prevention utilizing Amifostine, a radioprotector. Both research and clinical observation confirms that it dramatically reduces the incidence of severe xerostomia. Unfortunately, it is not universally employed by radiation oncologists due to side effects which include hypotension (low blood pressure), allergic reactions, and nausea.
Post Radiation
Patients are typically seen 4 months after completion of radiation therapy for dental cleaning, reinforcement of lifelong daily fluoride application, evaluation of both soft tissues of the mouth and the dentition. They are placed on a 3-4 month recall with the hygienist. Ability to open the mouth is evaluated. If it is restricted, trismus, therapy is initiated. The most common modalities are: tongue blade physiotherapy, Therabite®, Dynasplint®, warm heat, anti-inflammatory and muscle relaxant drugs.
Dental Treatments
Patients can have many dental procedures. Others are contraindicated. Special care must be taken. Restorative procedures such as fillings and crowns can be performed. However, many patients have difficulty swallowing and opening their mouths. Treatment tends to be slower and extra care should be taken to prevent /minimize aspiration. Endodontics (root canals) can be safely done. The fillings should not extend beyond the apices of the roots. Periodontics, gum treatment, should be limited to the non-surgical modality, i.e. deep cleaning in areas where the bone received a significant dose of radiation. Removable prostheses such as complete dentures and removable partial dentures are generally fabricated 6-24 months after completion of radiation treatment to minimize the breakdown of the soft tissue covering radiated jaw bone. Dental implant treatment can be accomplished in many cases. It involves interpretation of isodose maps (IMRT) and simulation films (external beam) to determine the radiation dose to the proposed implant sites. It may sometimes involve pre and post operative hyperbaric oxygen therapy to promote healing. Oral surgery, i.e. removal of teeth in areas of the jaw that have been radiated should generally be avoided due to the risk of osteoradionecrosis, a progressive non-healing wound. If the extraction of the teeth is required in areas that received a high dose of radiation, it is done in conjunction with hyperbaric oxygen therapy (HBO). Twenty or more HBO treatments or dives are done prior to surgery and 10 or more post surgically to assure normal healing.
The complications of exposed bone and osteoradionecrosis have become more common with the advent of combined chemotherapy and radiation therapies to treat cancer of the tongue, tonsil, and throat. The presence of exposed jaw bone several months after completion of treatment is quite common. Many times the body will shed it and the area will cover with soft tissue. A more ominous presentation is exposed bone that develops spontaneously or secondary to oral surgery several years after radiation therapy, i.e. osteoradionecrosis. Treatment consists of hyperbaric oxygen treatment which re-establishes microcirculation in conjunction with the appropriate surgical management.
Combined Radiation and Chemotherapy
Presently, the use of combined chemotherapy and radiation is routine for most of the locally advanced head and neck and oral cancers. Induction chemotherapy can be given prior to radiation. More commonly, it is given concomitantly with radiation therapy, i.e. combined therapy. The side effects tend to be the same as with radiation. However, they develop more rapidly and tend to be more severe. Additionally, chemotherapy causes immunosuppression. Oral infections such as candida and herpes simplex are quite common and must be treated. Dental treatment must be coordinated with the Medical Oncologist to insure that both the patient’s immune system and clotting factors will be adequate to fight infection and induce blood clot formation both during and following dental treatment.